A healthy nail plate is always transparent, colorless and its surface is smooth.Namely, thanks to the capillaries located under the nail plate, passing through it, it appears pink.But for some reason, white or yellow spots sometimes begin to appear in the thickness of the nail, which, as they increase, take the form of longitudinal grooves.Slowly moving from the free edge to the cuticle, they will gradually acquire an ocher-yellow color.Fungal damage to nails.Connecting with each other and increasing in size, they are able to capture the entire nail plate up to the posterior nail fold.Due to the development of horny masses in the nail bed area, the nail becomes thicker and the free edge of the nail may separate from the nail bed.Soon the shine of the nail disappears and the free edge becomes uneven.In some patients, the nail plate may separate from the bed, exposing a set of crumbling horny masses.The color of the affected nail plates varies from yellow-brown to gray.
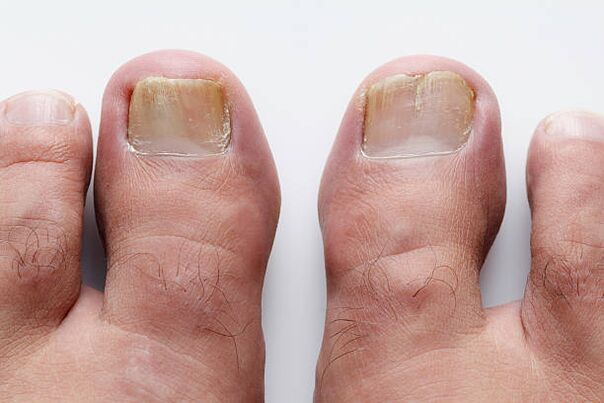
All of the described changes occur most often with onychomycosis.This term appeared in 1854 to designate nail lesions caused by pathogenic fungi.Onychomycosis is a fairly common nail disease;This occurs in 10 to 20% of people.Fungal foot infections are more common in countries with cold climates.But uncomfortable and tight shoes advantageously create conditions conducive to the development of infection, regardless of climatic conditions.The risk of getting onychomycosis increases with age, which is why onychomycosis is more often seen in older people.Sources of fungal infections are swimming pools, gyms, showers, common baths, locker rooms, dormitories, uncomfortable shoes that compress the foot, arterial or venous insufficiency, immunodeficiency, diabetes mellitus.And of course, you can get infected at a pedicure or nail salon.Hand onychomycosis, especially those caused by yeast-like fungi, is more common in women who keep their hands in water or soapy water for a long time, or who work with sugar, dairy products, or antibiotics.
In most cases, nails are affected by dermatophytes, quite often by yeast-like fungi and less often by mold.The main causative agents of onychomycosis are dermatophyte fungi.Their share is up to 90% of the total mass of fungal infections.The most common pathogens of onychomycosis are T. rubrum (about 80% of cases) and T. mentagrophytes var.Interdigital (10-20%).Typically, they first affect the spaces between the fingers, and then the nails themselves.It is therefore important to prevent skin infections.Candidiasis can be contracted through contact with foods high in carbohydrates.In addition, mold lives in the soil, therefore, the causative agent of mold onychomycosis is found in the external environment and often attaches to an already changed nail.Many scientists believe that this disease is less contagious.
The clinical division of onychomycosis is associated with the possible route of penetration of the fungus into the nail.Distinct lateral subungual, superficial white, proximal subungual and total dystrophic onychomycosis are distinguished.Most often, pathogenic fungi settle in the subungual space.From there, they can penetrate the nail bed.Under the influence of dermatophytes, the epithelial cells of the nail bed produce soft keratin, which, once accumulated, lifts the nail plate.Hyperkeratosis is characterized by a whitish color of the lesion.Soft keratin encourages the growth of fungi – a vicious cycle occurs.The nail plate, made of hard keratin, does not change at first, but later the dermatophytes create an aerial network of tunnels, and once this network becomes sufficiently abundant, the nail loses its transparency.Often the infection spreads along the longitudinal grooves of the nail.Infection of the matrix - the growth zone - by fungi causes various dystrophic changes in the nail.
Rubromycosis (caused by T. rubrum) affects the toenails and often the hands.More than 90% of patients experience increased dryness and increased keratinization of the skin of the hands and feet.While maintaining their shape and size, the nail plates can become covered with spots and stripes of white or yellow color.There is no discomfort associated with this disease and patients do not always notice these changes (normotrophic type).With the hypertrophic type, significant thickening of the nail plates is possible due to the accumulation of horny masses under them.They become dull and crumble easily.With such changes in the nail plates, patients often complain of pain in the toes pressed by shoes when walking.Nails affected by rubromycosis become noticeably thicker and curved, resembling bird claws (mycotic onychogryphosis).With the lesion of the onycholytic type, the nail plates become thinner and often, from the beginning of the process, separate from the nail bed from the side of the free edge.The separated part becomes dull and often acquires a dirty gray color.The proximal part of the nail, especially those located closer to the lunula, retains its natural color for a long time.On the exposed areas of the nail bed, layers of rather loose hyperkeratotic masses form.
Athlete's foot often develops in patients with excessive sweating of the feet.Athlete's foot most often begins on the free or lateral edges of the index or fifth finger.The causative agent of athlete's foot (T. mentagrophytes var. interdigitale) is one of the most aggressive fungal pathogens of infections of horny structures.
Yeast fungi Candida spp.representatives of normal human microflora.European studies show that Candida infection causes onychomycosis of the feet in 5 to 10% of cases and of the hands in 40 to 60% of cases.The disease occurs when the immune system is weakened and the normal composition of the microflora is disrupted.Candida onychomycosis develops more often in people suffering from diabetes mellitus, obesity and thyroid insufficiency.In case of candidiasis, redness and pain in the nail folds precede damage to the nail plates.Inflammation, change in shape and thickening of the ridges lead to separation of the cuticle from the surface of the plaque.As a result, fungi penetrate the nail matrix and from there penetrate into the nail plate and bed.Onychomycosis, associated with paronychia, is also seen in non-dermatophyte infections, for example streptococcal.
More than 40 types of mold are known, the causative agents of onychomycosis.Some of them are soil dwellers, present everywhere in the environment, and affect healthy nails.But most often already changed nail plates become infected.These changes can be caused by dermatophytes or result from one of several degenerative processes leading to deformation and, above all, disruption of the microstructure of the nail bed and the nail itself.
Onychomycosis, caused by mold, usually appears on the feet.The clinical picture may outwardly correspond to changes in various dermatoses, for example, psoriasis, which leads to diagnostic errors and ineffective treatment.It is therefore necessary to carry out laboratory tests.The affected part of the nail plate is treated with special solutions and examined under a microscope.The diagnosis is confirmed when mycelium filaments of a pathogenic fungus are detected.The type of pathogen is determined by growing a fungal culture on a nutrient medium.
Onychomycosis does not disappear spontaneously.If left untreated, the infection can quickly begin to affect nails one by one.For treatment, special external and systemic (oral) antifungal drugs are used.
Treatment of fungal nail infections
According to data, the nail plate of the hands grows by 2 to 4.5 mm per month, and that of the feet one and a half times slower.A complete nail plate on the hands can grow in 4-5 months, and on the feet in 11-17 months.Nails on different fingers grow at different rates;the nails of the big toes grow longer than the others.Since nails grow slowly, when analyzing the effectiveness of a treatment, it is not necessary to focus on the external condition of the nails;the result obtained can only be determined after receiving the results of microscopic tests and culture.Systemic antifungal agents should not be used more than recommended in the instructions if culture or microscopy results become negative.Otherwise, you can either continue treatment or change antibiotics.External therapy creates a protective layer on the surface of the nail, with a high concentration of antifungal agent.The main advantage of local therapy is safety, absence of toxic and side effects.
The disadvantage of local external treatment is the fact that the drug does not always reach the causative agent of the infection - the fungus located in the nail plate and matrix.To destroy the pathogen, the nail plate is removed or medications are prescribed to soften it.Medications used externally, for example, varnishes, can only be effective at an early stage.They are used for several months.When the nail matrix is damaged, local treatments for onychomycosis are ineffective.In addition, patients do not always systematically follow the doctor's instructions.If most nails are affected, systemic agents should be prescribed.
With a systemic approach to treatment, medications will penetrate the nail surface through the blood.Many of them accumulate in the matrix and remain there even after processing is complete.One of the limitations of systemic treatment is the development of side and toxic effects, for example hepatitis, associated with prolonged use of drugs for several months.Systemic treatment is not recommended for pregnant or lactating women, people with liver disease or drug allergies.Currently, modern antifungal drugs and progressive methods of their use have appeared, so the risk of side effects and toxic reactions has been significantly reduced.Although cases of ineffective therapy remain.Most often, they are associated with simultaneous infection of the nail plate with various types of pathogenic fungi, insufficient concentration of the drug in the nail plate (due to poor absorption of the drug in the patient's gastrointestinal tract, diabetes, obesity, poor blood circulation in the extremities) or non-compliance by the patient with the drug regimen.
When choosing a treatment, systemic or local, it is important to take into account all concomitant diseases, the body's resistance, the condition of the blood vessels of the extremities and metabolic characteristics.Without correcting your general well-being, it is very difficult to achieve rapid and quality results in the treatment of onychomycosis and avoid relapses and reinfections.
In order to reduce the incidence of onychomycosis, it is necessary to timely treat fungal skin diseases, not to wear someone else's shoes, to monitor the hygiene of the skin of the feet, to regularly visit the showers of gyms, swimming pools and similar establishments, and to use local antifungal drugs.It is necessary to maintain the cleanliness of common areas and carry out preventive examinations of staff and visitors.In manicure and pedicure rooms it is impossible to serve, let alone treat, patients with onychomycosis.Equipment needed for working with clients should be sterilized and disposable materials should be used whenever possible.


















